
Emily Greenstein, APRN, CNP, CWON, FACCWS is a Certified Nurse Practitioner at Sanford Health in Fargo, ND. She is certified as an Adult-Gerontology Nurse Practitioner through the American Academy of Nurse Practitioners. She has been certified in wound and ostomy care through the WOCNCB for the past 9 years. At Sanford, she oversees the outpatient wound care program, serves as chair for the SVAT committee, and is involved in many different research projects. Emily Greenstein is a paid consultant for Solventum.
Greenstein_Current-Dialogues-in-Wound-Management_2024_Article-4
INTRODUCTION: Chronic non-healing wounds affect an estimated 2% of the United States (US) population.1 However, the prevalence of chronic wounds has been increasing, affecting 16.4% of Medicare beneficiaries in 2019, a 13% increase from 2014.>2 In the acute wound care setting, 17.2 million hospitalizations for acute wounds were reported in the US for inpatient surgical and outpatient visits in 2014.1 With an increase in patients requiring wound care, development of new wound care options has also intensified. Negative pressure wound therapy (NPWT) acts by preparing the wound bed for closure, reducing edema, promoting granulation tissue formation and perfusion, and by removing exudate and infectious material. Randomized controlled trials have reported that NPWT leads to higher rates of wound closure, greater reduction in wound size, development of granulation tissue, and reduced times to closure and hospital length of stay for diabetic foot ulcers (DFUs), venous leg ulcers (VLUs), and pressure injuries compared to standard dressings.3 Recent meta-analyses have also reported a significant association between NPWT use and several positive outcomes, including granulation tissue development, increased healing rates, reduced wound sizes, and faster wound healing when compared to standard dressings for DFUs, VLUs, pressure injuries, and mixed chronic wounds.4 Traditional dressings for NPWT often require a long application process involving a multiple-step process of measuring and cutting foam, and adhesive components separately. Additionally, traditional NPWT dressings should be changed every 48-72 hours, but no less than 3 times per week, with frequency adjusted by the healthcare practitioner as appropriate.The new 3M™ V.A.C.® Peel and Place Dressing represents the next evolution in 3M™ V.A.C.® Therapy. It has an all-in-one
dressing and drape design that simplifies the application process and reduces the time required for dressing application. Additionally, this new dressing helps reduce the training required for both dressing application and changes. The V.A.C.® Peel and Place Dressing also features a built-in perforated, non-adherent layer that reduces tissue ingrowth and makes dressing removal less painful.The V.A.C.® Peel and Place Dressing is indicated for wounds as deep as 6 cm including chronic, acute, traumatic, subacute, and dehisced wounds, as well as partial thickness burns, ulcers (such as diabetic, pressure, or venous insufficiency), flaps, and grafts. The V.A.C.® Peel and Place Dressing can reduce therapy application time by 61%, reduce costs by 41% due to less frequent dressing changes, and reduce the number of home nursing visits by 67% per week.6 A simulated use test with 12 nurse and surgeon users compared dressing application times between V.A.C.® Peel and Place Dressing and traditional NPWT foam dressing with hybrid acrylic-silicone drape. The V.A.C.® Peel and Place Dressing took an average of 1:48 minutes to apply, whereas the traditional NPWT foam dressing and hybrid acrylic-silicone drape took an average of 4:40 minutes to apply (p<0.01).5 The novel V.A.C.® Peel and Place Dressing is a combination of the reticulated open cell foam and the 3M™ Dermatac™ Drape, an advanced silicone-acrylic hybrid drape. Dermatac Drape provides wound healing support for patients receiving 3M™ V.A.C.® Therapy with the dual benefits of high-tack acrylic adhesive and forgiving silicone. Dermatac Drape is strong enough to maintain a negative pressure seal, yet gentle enough to help lessen or remove pain during dressing changes. Additionally, Dermatac Drape can be repositioned during the initial placement allowing the clinician to easily smooth wrinkles without the loss of adhesion. A recent study has shown that patients managed with NPWT and the hybrid drape showed no periwound skin irritation or other complications, indicating that the hybrid drape can be used with minimal complications.7
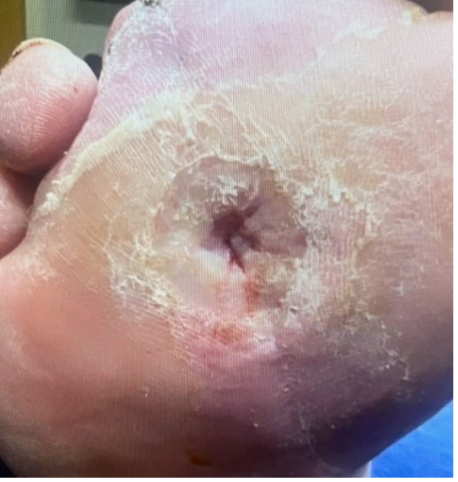
Case Report:A 56-year-old male with a history of type 2 diabetes who was treated for a diabetic foot ulcer on the plantar surface of the right foot at a rural wound care center (Figure 1). The patient had previously undergone a transmetatarsal amputation on the right foot. He was undergoing hyperbaric oxygen therapy daily. Previous wound care included advanced topical dressings along with offloading of the area. The ulcer had been present for greater than 90 days when the V.A.C.® Peel and Place Dressing was applied. The decision to apply the V.A.C.® Peel and Place Dressing was made because the wound was difficult to heal and would benefit from NPWT. However, the small size of the wound made traditional NPWT application cumbersome, as the dressing application would be complicated and require extensive cutting and draping to obtain a seal. The patient would also be at high-risk for periwound skin breakdown due to the location of the wound.
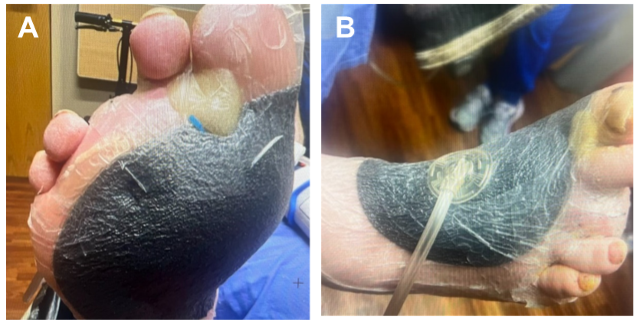
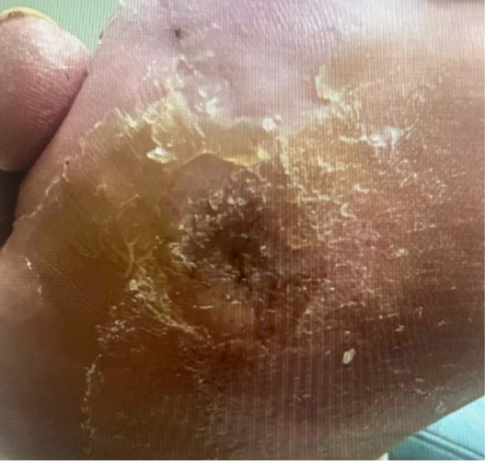
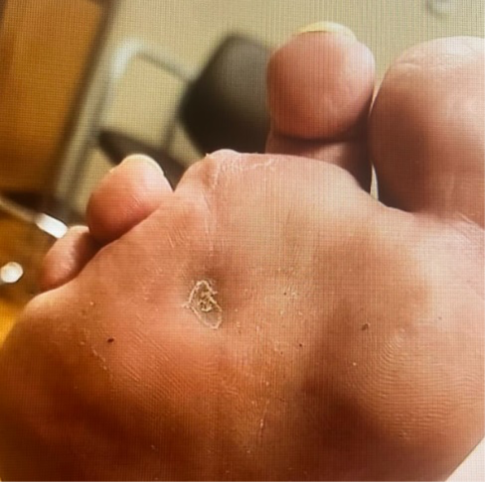
The V.A.C.® Peel and Place Dressing was applied using the large size dressing, connected to the 3M™ ActiV.A.C.™ Therapy Unit, and -125 mmHg negative pressure initiated (Figure 2). The large dressing size was chosen to allow for bridging to the dorsal foot surface and prevent potential pressure injuries due to 3M™ SensaT.R.A.C.™ Pad and tubing. A hydrocolloid ring was also placed between the toes to help achieve a negative pressure seal in this difficult anatomical area. Dressing application was quick and easy, taking approximately 5 minutes. Throughout the use of NPWT, the negative pressure seal remained intact. After 7 days of NPWT, the wound was fully healed (Figure 3). Dressing removal on day 7 was painless and the periwound skin was intact without any irritation. The wound remained healed at the 21-day follow-up visit (Figure 4).
CONCLUSION: This case demonstrated the use of V.A.C.® Peel and Place dressing on a diabetic foot ulcer. The dressing offered several advantages over the traditional reticulated open cell foam dressings including decreased application time, increased wear time, and fewer appointments for the patient. The advanced dressing used a hybrid silicone and acrylic drape allowing for protection of the periwound skin, even though the dressing was left in place for 7 days. The new V.A.C.® Peel and Place Dressing is an excellent addition to any wound care toolbox.
References
1. Sen CK. Human wounds and its burden: updated 2020 compendium of estimates. Adv Wound Care (New Rochelle). 2021;10(5):281-292. doi:10.1089/wound.2021.0026
2. Carter MJ, DaVanzo J, Haught R, Nusgart M, Cartwright D, Fife CE. Chronic wound prevalence and the associated cost of treatment in medicare beneficiaries: changes between 2014 and 2019. J Med Econ. 2023;26(1):894-901. doi:10.1080/13696998.2023.2232256
3. Hemkens LG, Waltering A. Comparison of negative pressure wound therapy using vacuum-assisted closure with advanced moist wound therapy in the treatment of diabetic foot ulcers: a multicenter randomized controlled trial: response to Blume et al. Diabetes Care. 2008;31(10):e77. doi:10.2337/dc08-0890
4. Liu S, He CZ, Cai YT, Xing QP, Guo YZ, Chen ZL, et al. Evaluation of negative-pressure wound therapy for patients with diabetic foot ulcers: systematic review and meta-analysis. Ther Clin Risk Manag. 2017;13:533-544. doi:10.2147/tcrm.S131193
5. 3M™ V.A.C.® Peel and Place Dressing Kit. SAT-MTF-05-995965 Marketing study for 3M V.A.C. Peel and Place dressing. 2023.
6. 510(k) K222859 [V.A.C. Peel and Place dressing]; SAT-TEST-RPT-05-893424 Ganymede FDA System Test 2022 [V.A.C. Peel and Place dressing]; SAT-TEST-RPT-05-794416 FDA System Functional Test Report [V.A.C./Dermatac/Granufoam system] 72 hr performance test. 2022.
7. Greenstein E, Moore N. Use of a novel silicone-acrylic drape with negative pressure wound therapy in four patients with periwound skin breakdown. Wounds. 2021;33(1):304-307. doi:10.25270/wnds/091421.01
NOTE: Specific indications, contraindications, warnings, precautions and safety information exist for these products and therapies. Please consult a clinician and product instructions for use prior to application. Rx only.
As with any case study, the results should not be interpreted as a guarantee or warranty of comparable results. Individual results may vary depending on the patient’s circumstances and condition.
Patient data and images courtesy of Emily Greenstein, APRN, CNP, CWON-AP, FACCWS.
© Solventum 2024.

